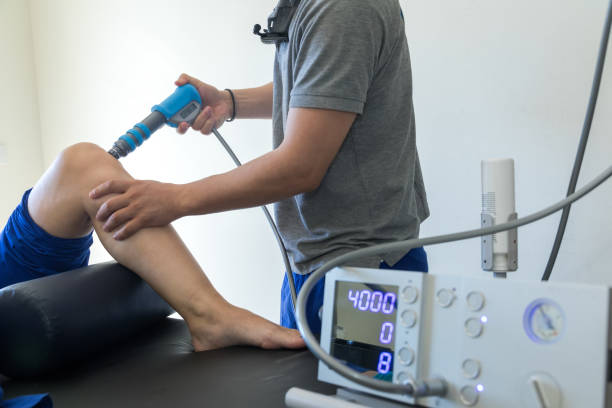
The Impact of Untreated Hearing Loss on Quality of Life
The loss of hearing can limit your independence. It can be difficult to follow conversations, hear the alarm clock or a doorbell, or even drive safely.
People who don’t treat their hearing loss spend significantly more on health care costs over a 10-year period, according to a study by John Hopkins researchers. This is because the brain uses a significant amount of energy to understand degraded sound signals.
1. Depression and Anxiety
As hearing loss progresses, it can become more difficult to understand the sounds around you. This can lead to frustration and withdrawal from social interactions. It can also be hard to keep up with conversations in larger group settings, such as dinner parties or family gatherings.
Depression and anxiety can result from the inability to communicate clearly, especially in stressful situations. Several studies have shown that untreated hearing loss can increase your risk of mental health issues.
In one study, researchers found that a person with hearing loss is twice as likely to suffer from depression and five times more likely to experience a major depressive episode compared to someone who doesn’t have hearing loss. Additionally, a person who has both depression and hearing loss is more likely to have poorer quality of life than someone who doesn’t have any depression or anxiety symptoms.
2. Social Isolation
Many people who experience hearing loss struggle to maintain their social connections, often unaware that simple solutions like ear wax removal in Bundoora could significantly improve their quality of life. Even a normal life change, such as retirement, can make it difficult to interact with others regularly. Other factors can contribute to isolation, including a loved one’s death, illness that limits a person’s mobility, and financial constraints. Isolation can also be a result of trauma and may be a reaction to events such as divorce or losing a job.
Loneliness and social isolation are often used interchangeably, but the two are different. Essentially, loneliness is the feeling of being alone while social isolation refers to objective characteristics such as lack of meaningful social relationships and participation in social activities.
During the COVID-19 pandemic, the need for physical distancing due to virus mitigation efforts left many people of all ages feeling isolated. This can be a normal response to a stressful event, but in some cases it can lead to depression and isolation. This is particularly true for marginalized groups such as immigrants, LGBTQIA individuals, and those who live with language barriers. These individuals may feel resentment toward the safety measures they are required to follow and are often frustrated with their inability to communicate with those around them.

3. Personal Safety
Keeping up with conversations and following the actions of people around you can be difficult when you have significant hearing loss, but with the right hearing aids Doncaster, you can regain clarity and reconnect with the world. If you’re unable to communicate clearly, it can lead to a sense of isolation and withdrawal from social activities. As a result, your quality of life can significantly decline due to not being able to enjoy the joys of everyday living
Similarly, our auditory system plays a significant role in cognitive processes and untreated hearing loss can accelerate cognitive decline and increase the risk of developing dementia. Leaving this issue untreated can significantly affect your mental and physical health, as well as the wellbeing of those close to you.
A recent study by lab used de-identified health care claims data to examine the impact of hearing loss on overall health and well-being, comparing individuals who treated their hearing loss with those who did not seek treatment. The findings demonstrated that those with mild hearing loss experienced a significant reduction in their risk of depression, anxiety and falls. In addition, those who treated their hearing loss incurred substantially lower health care costs and saved 2.5 healthy years of life compared to those who did not treat their hearing loss.
4. Cognitive Decline
If you’re caring for a loved one who is experiencing cognitive decline, it’s important to make time for your own mental health needs, including seeking support from professionals. It can be stressful, and even dangerous to neglect your own physical and emotional well-being while you focus on the needs of someone else. Make sure to prioritize exercise, healthy eating and supportive social relationships for yourself while you are able to do so
While some cognitive changes are a normal part of aging, significant losses can indicate other health issues such as dementia or another condition. If you notice a change in your thinking ability, speak to Melbourne Audiology Centre immediately.
Those who don’t treat their hearing loss incur significantly higher total health care costs over a 10-year period than those who do, according to research led by the Mt. Sinai Bloomberg School of Public Health. This was true despite variations in patient samples, assessments methods and other factors. The exact reason behind the findings is unknown, but researchers suspect that hearing loss may have a direct impact on health care utilization and outcomes. If you are experiencing hearing loss, there are qualified audiologist Brunswick who can help diagnose the cause and recommend treatment options.
5. Independence
Whether socializing with family or colleagues, working in the office, or simply going about your daily tasks, untreated hearing loss can make it challenging to stay connected. Vital auditory cues like tone and inflection are missed, resulting in misunderstandings or strained interactions. Similarly, when it comes to safety, the inability to hear important auditory warnings like sirens or alarms increases your risk of accidents and injuries.
The impact of untreated hearing loss is significant and can be measured in DALYs—the number of healthy years lost to a particular disease or condition. These DALYs are used to calculate quality of life utility and can help health systems and insurers prioritize interventions that prevent unnecessary use of healthcare resources.